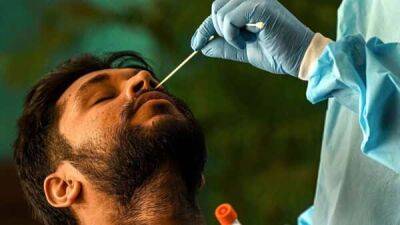
Initial vital signs, labs better predict COVID severity than chronic conditions
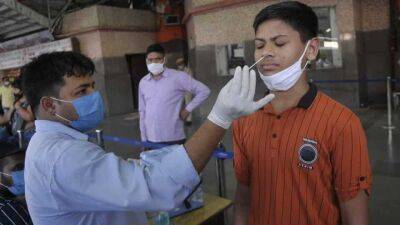
COVID-19 patients' vital signs, lab results, and need for supplemental oxygen when they arrive at the hospital can better predict illness severity than underlying illnesses and differ by age-group, suggests a modeling study published today in Scientific Reports.A team led by Institute for Systems Biology in Seattle led the study to improve risk stratification for hospitalized COVID-19 patients, a process important for clinical decision-making and resource allocation.Delta dominated study periodThe researchers retrospectively analyzed the electronic health records from 6,906 adults hospitalized with COVID-19 from a community health system with 51 hospitals and 1,085 clinics in Alaska, California, Montana, Oregon, and Washington from Jun 30 to Nov 15, 2021, a period dominated by the Delta SARS-CoV-2 variant.
Most hospitalized patients (92% of those younger than 50, 75% of older patients) hadn't been vaccinated against COVID-19.Using clinical data from the first hour of either hospital admission or positive COVID-19 test, the team built models to predict the need for mechanical ventilation or death in the next 56 days.
Patients were classified as younger than 50 years (1,963 patients) or 50 and older (4,943). Average patient age was 60 years, and 44.3% were women.Aggregated vital sign values from 24 hours before to 1 hour after included average heart rate, systolic and diastolic blood pressure, respiratory rate, blood oxygen saturation, and body temperature.The risk-prediction models for within 7 days of hospitalization or diagnosis had an under-the-receiver operating characteristic (AUROC) of 0.81 for younger patients and 0.82 for the older group, indicating excellent performance.Critical illness or death occurred in 10.9%