Infection preventionists' mental, physical health suffered in pandemic
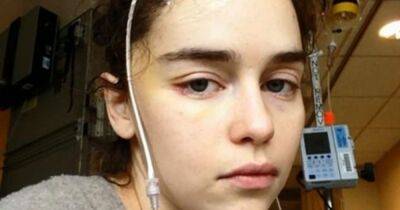
High percentages of infection preventionists (IPs) reported that COVID-19–related stressors worsened their mental and physical health, highlighting the need to address systemic issues that lead to burnout and improve recruitment and retention, according to survey results reported yesterday in the American Journal of Infection Control.In the first-of-its-kind study, researchers from Ohio State University and the Association for Professionals in Infection Control and Epidemiology (APIC) emailed a survey to a random sample of 6,000 APIC members on issues surrounding mental and physical well-being, lifestyle behaviors, and perceived workplace wellness support during COVID-19.Participants also answered questions on three questionnaires: the Patient Health Questionnaire-2, the Generalized Anxiety Disorder-2, and the Professional Quality of Life.Most respondents (93.5%) were women, aged 35 to 64 years (77.1%), White (86.8%), married or in a relationship (82.5%), held a bachelor's (41.2%) or master's (42.3%) degree, worked 9- to 10-hour shifts (58.2%), worked in hospitals (68.1%), were not current smokers (92.1%), and were light drinkers (69.3%).Amid the pandemic, IPs have had to adapt to rapidly evolving infection-prevention recommendations, shortages of personal protective equipment, increased hospital-acquired infections, and heavier workloads, the authors noted.Only 17% report high quality of lifeOf the 6,000 invitees, 926 (15%) completed the survey.
About two-thirds indicated they were in good physical (68.9%) and mental health (66.0%). But respondents reported low rates of getting at least 7 hours of sleep a night (34.1%), being physically active for at least 150 minutes a week (18.8%), and eating five or more servings of